If Your Glaucoma Is Being Treated — But Your Vision Is Still Getting Worse — This Page Explains Why
Written for people who have a confirmed glaucoma diagnosis, are already doing what their doctor recommended — and are still watching their vision slowly change. If that's not your situation, this page probably isn't for you.
A physician with 14 years treating advanced vision loss recently recorded this. It's not what most patients expect to hear:
Free to watch · No sign-up · ~12 minutes
If you've been diagnosed with glaucoma and you're following your treatment plan — using your drops, going to your appointments, monitoring your pressure — you're doing what you're supposed to do.
And yet, for many people in exactly that situation, something quietly changes. The side vision gets a little narrower. Night driving becomes harder. Faces across a room become harder to make out.
The pressure numbers might be fine. The doctor says things are stable. But you can feel that something is different. And that feeling doesn't go away.
This page is specifically for people in that situation. If you don't have glaucoma, or if your condition has been completely stable and you have no concerns — you're probably not going to find this relevant. But if the description above sounds familiar, keep reading.
Glaucoma doesn't take your sight all at once. That's what makes it so hard to deal with emotionally. It removes it gradually — a little at a time, mostly from the edges — until one day the absence of something you used to have becomes undeniable.
You start turning your head more when you drive. You avoid going out at night. You find yourself asking someone to read something you used to read on your own. And there's a specific moment — one that many people with glaucoma describe — when they realize they can no longer clearly see the face of someone they love from across a room.
"The part that scared me most wasn't the idea of going blind. It was realizing I was already starting to depend on other people for things I'd always done myself — and no one had warned me that could happen while my pressure was still 'controlled.'"
That's the reality for a significant number of glaucoma patients: they manage the measurable numbers faithfully, and still lose meaningful vision. Not because they did anything wrong. Because something else is happening — something the standard treatment wasn't designed to address.
- Peripheral vision gradually narrowing — even with controlled pressure
- Night driving becoming unsafe — headlights feel overwhelming
- Difficulty recognizing faces from a distance — and hoping others don't notice
- Needing help with labels, signs, or screens you used to manage easily
- Using prescription drops consistently — and still watching things change
Only relevant if you're already diagnosed and noticing changes.
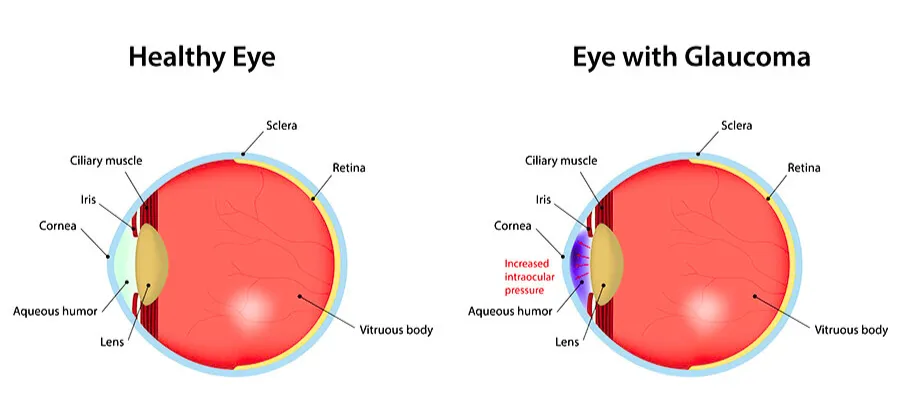
Most glaucoma treatment is built around a single goal: reduce intraocular pressure to a target range. And that's genuinely important. Elevated pressure does damage the optic nerve over time. No one is disputing that.
But here is something that rarely gets discussed in a clinical appointment: pressure and vision loss do not always move together.
There are patients with consistently well-controlled pressure whose visual field continues to shrink. There are others with elevated pressure who go years without meaningful progression. This inconsistency is well-documented in the ophthalmology literature. Researchers have known about it for decades.
What it suggests is that something else is contributing to optic nerve damage — something that a pressure number doesn't measure, and that eye drops aren't designed to treat.
The question most patients never get to ask — because appointments are short, and the protocol is clear — is: what is that something else?
Over the past several years, a number of independent research programs have been investigating exactly this question. And the direction their findings point is not what most patients expect.
The emerging evidence suggests that the eyes — the optic nerve in particular — accumulate a different kind of damage over time. One that comes not from pressure, but from what they're exposed to every day: modern light sources, environmental toxins, compounds that enter the body through food, water, and air, and never fully leave.
This isn't the kind of damage that shows up in a pressure reading. It's quieter. Slower. And it appears to interfere with the eye's own natural ability to repair itself at the cellular level.
"The optic nerve does have a limited regenerative capacity. What researchers have been trying to understand is why that system appears to fail in so many glaucoma patients — even when their pressure is managed."
There's more to this — but explaining it fully would take longer than this page allows. What's relevant here is this: a physician who has spent over a decade working specifically on cases where conventional glaucoma management had reached its limits recorded a presentation explaining what his team found. And what they did about it.
Not for everyone — but relevant if your vision has been changing despite treatment.
Clinical Reference: A study conducted in collaboration with researchers at Harvard Medical School and reviewed by specialists at the Wilmer Eye Institute at Johns Hopkins followed over 550 patients with serious vision conditions — including glaucoma, macular degeneration, and diabetic retinopathy. The researchers examined whether certain naturally occurring compounds could influence the eye's cellular repair activity. The results were described by the lead investigators as unexpected. They are explained in detail in the video below.
A separate 5-year study by the National Eye Institute — following more than 4,000 adults between the ages of 58 and 86 — found a statistically significant relationship between specific antioxidant levels in the body and the rate of glaucoma progression. People with higher levels showed measurably slower deterioration.
These aren't fringe findings. They appear in peer-reviewed journals. But the distance between what researchers publish and what reaches a patient in a 15-minute clinical appointment is significant. And for people with glaucoma, that gap has real consequences.
The physician in this video has spent over 14 years treating patients with advanced, progressive vision loss — many of whom came to him after being told that further decline was inevitable. He isn't selling anything in the presentation. He's explaining a pattern he observed in his own clinical practice: patients who began addressing something the standard protocol wasn't targeting — and who experienced outcomes their previous doctors hadn't anticipated.
He's careful with his language throughout. He does not claim to cure glaucoma. He does not promise results. He explains what the research shows, what his patients experienced, and what he now recommends to people in situations like yours.
The people who find this video most useful are those who are already following their treatment plan — and still feel like they're losing ground. If that's where you are, it's worth 12 minutes.
For people with glaucoma whose vision is still changing
If Your Vision Has Been Getting Worse Despite Treatment — Watch This Before Your Next Appointment
This video won't ask you to stop your current treatment or make any promises. It will show you something specific — something most glaucoma patients in your situation were never told — and let you decide if it changes anything.
Watch the Short Video Now → Free · No sign-up required · Approx. 12 minutesIf your glaucoma is completely stable and you have no ongoing concerns, this video probably won't add anything for you. But if you've been noticing changes — even small ones — it's worth the time.